- Home
- La scuola
- Area Formazione
- Collegio Italiano dei Senologi
- Area donne
- Contatti
All’inizio degli anni 80 dalla ricerca, dopo decenni di sostanziale stagnazione, cominciarono finalmente ad arrivare idee e risultati che prefiguravano nuove e ben più efficaci possibilità di cura per i tumori della mammella. Favorire l’aggiornamento medico per consentire il rapido trasferimento di questi risultati nella pratica clinica quotidiana divenne quindi un’esigenza prioritaria ed è per questo che, fortemente pensata e voluta da Umberto Veronesi, il 19 aprile 1984 nacque con la firma dell’atto costitutivo la nostra Scuola.
Da allora abbiamo realizzato quasi 2000 eventi didattico-formativi a cui hanno partecipato decine di migliaia di professionisti fra medici, infermieri, tecnici di radiologia e psicologi. Siamo stati presenti in più di 150 città e collaborato con alcune delle più prestigiose Università, Società Scientifiche e strutture sanitarie nazionali.
Poiché non è certo questa la sede per tracciare un bilancio dettagliato di questi “primi 40 anni” voglio qui solo limitarmi a ringraziare tutti coloro che ci hanno sostenuto ed in particolare i nostri docenti che con competenza e passione ci hanno permesso di portare avanti l’attività senza condizionamenti e in totale indipendenza culturale. Attività che vogliamo continuare con l’entusiasmo di sempre come emblematicamente dimostra l’inaugurazione di una nuova edizione del Master in Ecografia Senologica avvenuta proprio oggi, giorno di questo per noi significativo compleanno, presso l’Ospedale San Carlo di Nancy a Roma.
Claudio Andreoli – Direttore

– Dal 10 maggio sono disponibili online i programmi definitivi dei corsi validi come parte teorica del “Master in Ecografia Senologica” che si terranno nella sessione autunnale a Milano, Palermo e Roma. Per informazioni e modalità di partecipazione clicca qui
– Programma definitivo della sessione di settembre (26-27-28) di “Building Bridges: the fully digital meeting in clinical oncology”. Evento patrocinato dalla Scuola Italiana di Senologia
 Qui è possibile trovare tutte le informazioni utili per poter partecipare agli eventi in programmazione (calendario, programmi, docenti e modalità d’iscrizione), consultare una rassegna della letteratura senologica internazionale aggiornata trimestralmente e avere un panorama delle novità editoriali in ambito senologico.
Qui è possibile trovare tutte le informazioni utili per poter partecipare agli eventi in programmazione (calendario, programmi, docenti e modalità d’iscrizione), consultare una rassegna della letteratura senologica internazionale aggiornata trimestralmente e avere un panorama delle novità editoriali in ambito senologico.
Calendario eventi in programmazione 2024
Master e percorsi di alta formazione
AIS – Attualità in Senologia: rassegna della letteratura
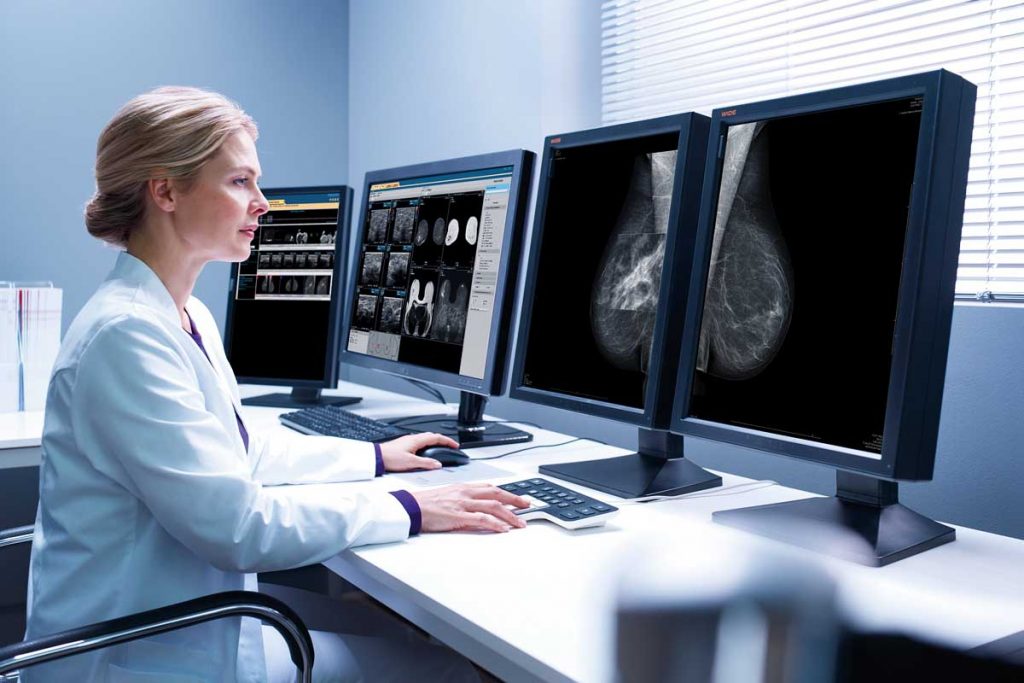
La Scuola, da oltre trent’anni impegnata a favorire la crescita professionale degli specialisti in radiologia che si dedicano alla senologia, propone una prova di refertazione mammografica, sviluppata e validata dal Consiglio Scientifico, basata su un campione significativo di esami eseguiti in donne asintomatiche sia nella pratica clinica quotidiana che in ambito di screening.
Il test fornisce un risultato in termini di autovalutazione mediante la stima della sensibilità e delle specificità a partire da una valore soglia determinato mediante validazione dello stesso test da parte di un campione di esperti (gold standard). Il raggiungimento di un punteggio soglia consente il rilascio di una certificazione di accuratezza diagnostica in mammografia. Leggi di più
“Ho voluto il Collegio perché credo che per un medico certificare la propria competenza in una disciplina così complessa come la Senologia sia un dovere verso le donne”. Umberto Veronesi

Il Collegio nasce nel 2012 per riunirvi i medici che dedicandosi alla cura della patologia mammaria dimostrano di avere e mantenere un elevato livello di aggiornamento professionale che permette di applicare con tempestività nella loro pratica clinica quotidiana le innovazioni della ricerca e garantire così alle pazienti i migliori trattamenti disponibili. Leggi di più
Regolamento e richieste di ammissione
Elenco Membri Certificati
I documenti del Collegio per la miglior pratica clinica
Nel corso degli anni molte delle nostre attività sono state rese possibili grazie alla collaborazione con alcuni dei più importanti Istituti Scientifici e Universitari italiani. Così come numerose Amministrazioni Pubbliche, Assessorati Regionali alla Salute ed Associazioni di Pazienti sono stati nostri partner in progetti di divulgazione scientifica volti a far crescere la cultura della prevenzione oncologica nella popolazione in generale e in particolare nelle persone più fragili (donne anziane, disabili, immigrate, detenute). Solo per citare due delle più recenti collaborazioni ricordiamo qui quella con All.Can International, organizzazione senza scopo di lucro multi-stakeholder che lavora per migliorare l’efficienza dei piani e delle politiche nazionali in ambito oncologico e quella con EUBREAST Study Group.
Sondaggio sulla formazione dei Senologi in Europa? European Union of Medical Specialists (UEMS-Multidisciplinary Joint Committee Breast Care) e European Breast Cancer Research Association of Surgical Trialists (the EUBREAST Network) promuovono un sondaggio aperto agli specialisti che si dedicano allo studio e alla cura dei tumori della mammella (radiologi, radioterapisti, patologi, chirurghi senologi, ginecologi, e oncologi) con l’intento di realizzare un quadro internazionale che faccia emergere l’eterogeneità in questo ambito. La Scuola Italiana di Senologia aderisce a quest’iniziativa e invita i medici che l’hanno frequentata a rispondere alcune domande sulla loro formazione a questo link.

Promuovere la consapevolezza che il tumore al seno può essere vinto grazie a una alleanza virtuosa fra medici e donne é sempre stato un nostro obbiettivo prioritario. Per far crescere nella popolazione la cultura della prevenzione abbiamo organizzato centinaia fra conferenze, incontri e dibattiti pubblici in tutto il territorio nazionale, offerto consulenze online gratuite, promosso campagne per la diagnosi precoce con visite senologiche, mammografie ed ecografie, prodotto e distribuito opuscoli e altro materiale informativo. Quest’Area del sito è un ulteriore strumento che mettiamo a disposizione delle donne italiane per informarsi, capire, fugare dubbi e perplessità ed aggiornarsi sulle nuove possibilità di diagnosi e cura.
Hai domande sul tumore al seno: scrivici qui!
“Paziente Diplomata” conferenza per donne con e senza tumore al seno: tutti i video
Tumore al seno: conoscere per vincere
Impareggiabile Maestro e caro Amico,
sono trascorsi ormai alcuni anni da quando te ne sei andato lasciando in tutti noi, che abbiamo avuto la fortuna di starti vicino e lavorare al tuo fianco, un vuoto davvero incolmabile. Ci hai sempre spronato a credere nel valore della scienza, della ricerca e dello studio. Ci hai dimostrato quanto l’empatia sia importante nel rapporto con i pazienti (ricordo che un giorno mi dicesti: vedi il sorriso è una medicina straordinaria, non costa nulla ma agisce tanto).

Ci hai insegnato la solidarietà, il rispetto per gli altri e per gli animali e tante, tante altre cose ancora. Ci hai però anche costretti, per anni, ad alzarci all’alba nell’illusoria speranza di riuscire ad arrivare in reparto o in sala operatoria prima di te ma tu, immancabilmente, eri già lì e questa è davvero l’unica cosa che non so se riuscirò mai a perdonarti.
Ti saluto qui nella Home della Scuola che hai voluto, fondato, sostenuto e amato certo che il tuo ricordo sia sempre ben vivo nella mente e nel cuore, non solo delle migliaia di pazienti che hai curato e a cui hai restituito la speranza, ma anche dei moltissimi medici che, come me, con i tuoi insegnamenti hai contribuito a rendere migliori.
Claudio Andreoli